Fertility Treatments
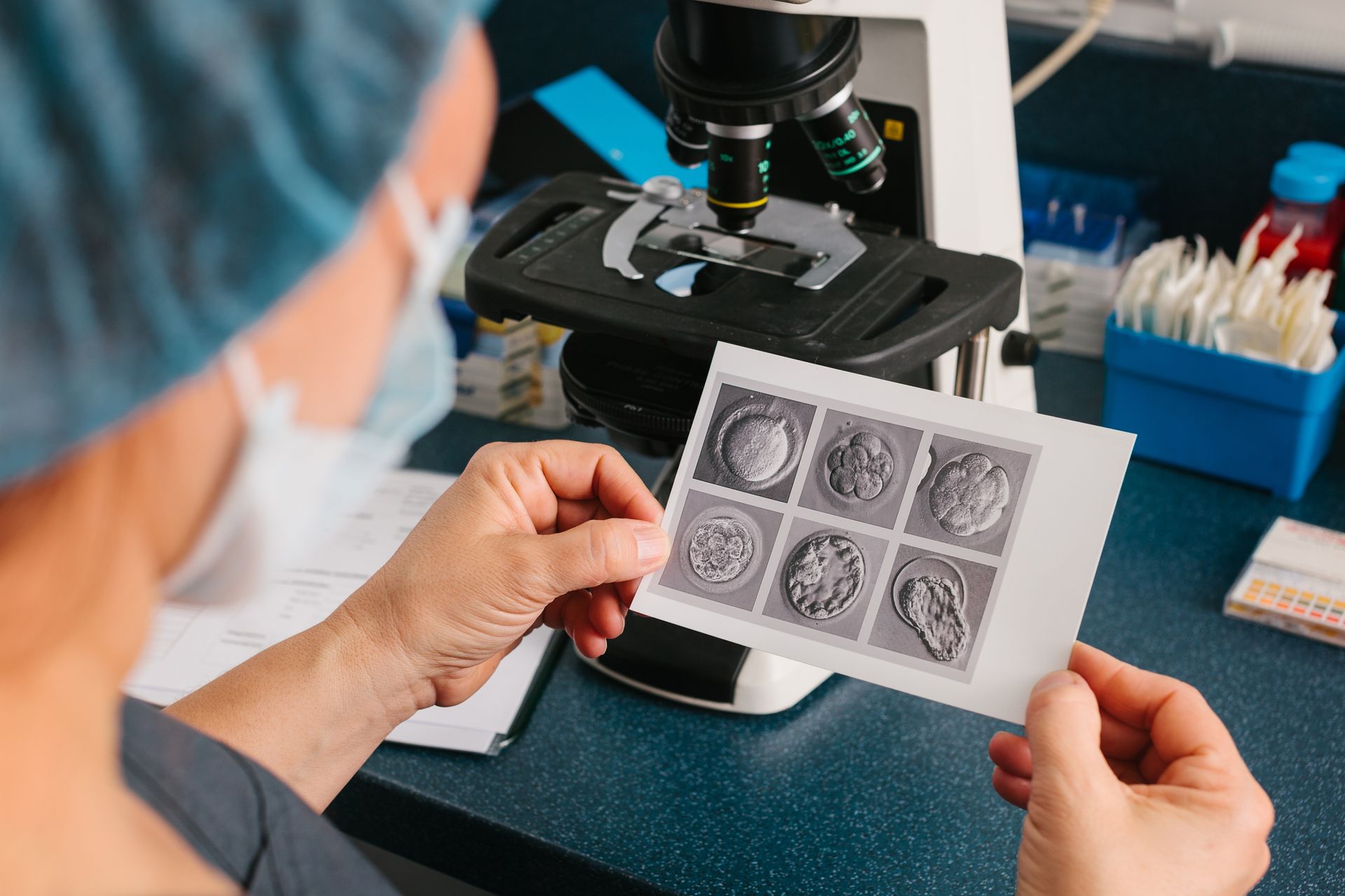
Conceptia offers a comprehensive range of fertility treatments to assist those experiencing fertility challenges across the Atlantic provinces.
We believe that because every situation is unique, every patient’s treatment plan should be customized based
on their needs, goals and the results of their assessments. Treatments range in complexity from simple
interventions to more advanced assisted reproductive technologies like IVF.
Explore treatments
Intrauterine insemination (IUI)
Intrauterine Insemination (IUI), also known as artificial insemination, is a common fertility treatment that consists in the insertion of washed sperm into the uterus. Because the steps necessary for natural conception occur in a IUI, it is often considered a less invasive procedure than other treatment options.
The IUI Steps
Preparing the sperm
The partner or donor semen sample is obtained or thawed on the morning of the IUI. It then undergoes washing in our laboratory in order to get rid of seminal fluid and to obtain a concentrated population of high quality sperm.
Insemination
The physician inserts a small, flexible catheter through the patient’s cervix and into her uterus, in a rapid and painless insertion. We recommend that patients arrive with an almost full bladder to facilitate insertion. The patient can resume activities within minutes, with light spotting being common. A blood pregnancy test is performed a couple of weeks after insemination.
Reasons for recommending IUI

Using a partner's sperm
Our medical team can recommend an IUI using a partner’s sperm in cases of mild male factor infertility (identified by fluctuations in sperm count, movement or shape). This can also be used in cases of unexplained or cervical factor infertility, females experiencing mild endometriosis, or repeated unsuccessfulness in conceiving despite ovarian stimulation
Using a Donor's Sperm
IUI can be explored for single women, same-sex female couples or couples with severe male-factor infertility. Our team may also discuss such a treatment with you if there is a history of certain genetic disorders in your family. There are four Health Canada-authorized distributors that can sell sperm samples, and they are required to rigorously inspect donors.
Find out more information about requirements and possibilities concerning donors.
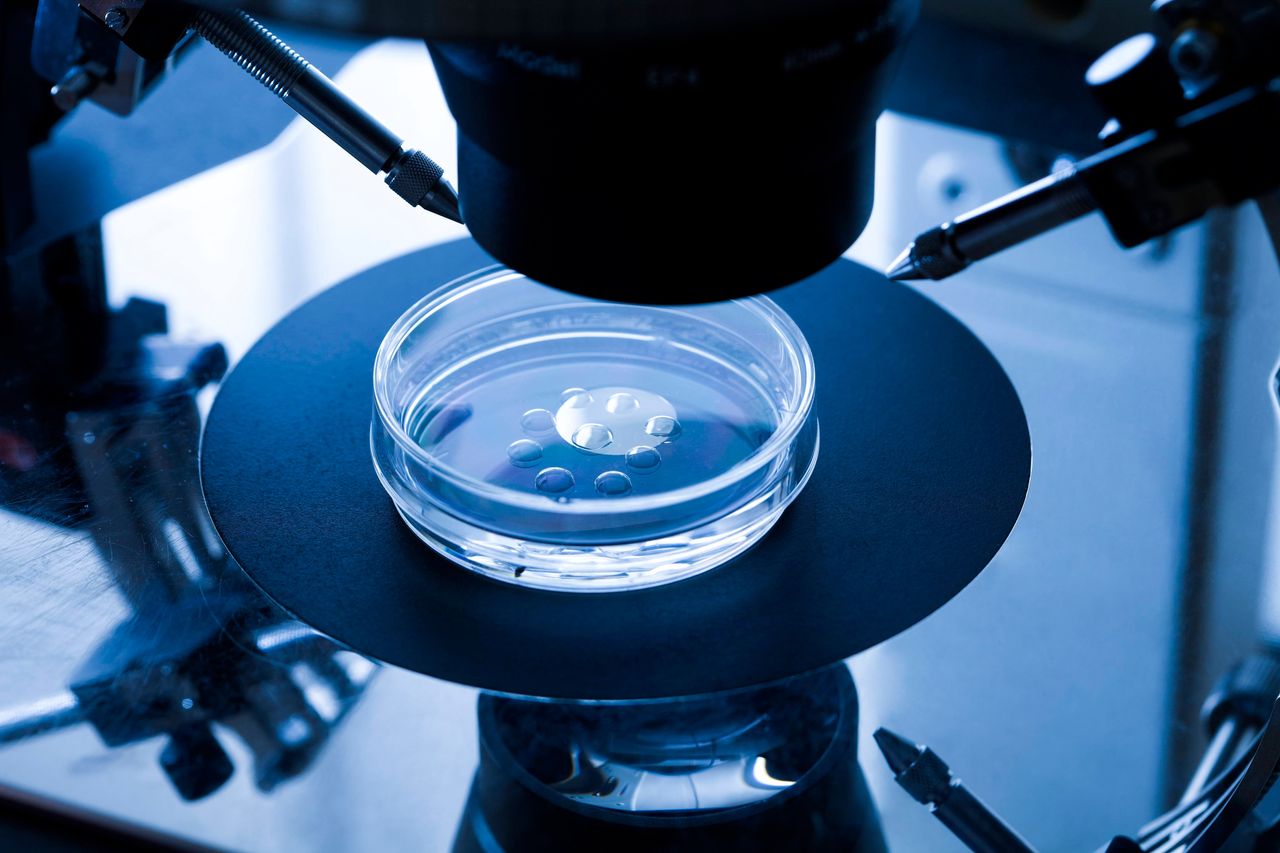
Ovulation Induction (Superovulation)
Ovarian induction
Ovarian induction (or stimulation) is a non-invasive technique that can be recommended by our medical team, especially if you and your partner are young and there is no obvious reason preventing you from conceiving. The objective of ovarian stimulation is to produce the maturation of two to three follicles (each containing a mature egg) instead of the one of regular menstrual cycles.
Before ovarian stimulation begins, blood work will be conducted to check for hormone level, as well as endovaginal ultrasounds, to examine the ovaries and the endometrial lining. Those tests are repeated in order to follow the progress of the ovarian stimulation.
Ovulation predictor kits
The purpose of this test is to detect an increase of luteinizing hormone (LH) in the urine, which is a sign of upcoming ovulation. Ovulation predictor kits (also known as LH kits) are therefore used to determine the ideal time to do the IUI. This test is similar to a urinary pregnancy test and can be purchased in most pharmacies.
In Vitro Fertilization (IVF)
In Vitro Fertilization (IVF) refers to a laboratory procedure in which mature eggs are exposed to sperm outside of the female body, in order to produce an embryo. This is distinct from IUI, in which the insemination is done into the female’s uterus. Your physician will determine whether IVF is the appropriate treatment in your fertility journey. IVFs can, for instance, be recommended to patients with blocked or nonfunctional fallopian tubes, advanced age, decreased ovarian reserve, or when other less invasive treatments have not been successful.
Understanding the phases in the IVF process
Ovarian and Uterine Preparation
During the first phase, you take medication to suppress the production of eggs and drop estrogen levels, which can be necessary to establish control over the patient’s cycle. Following this phase of ovarian suppression, the ovarian stimulation phase begins, in which you take medication to boost the production of eggs. In a typical menstrual cycle, a single egg is produced, but ovarian stimulation allows for the creation of multiple eggs per cycle, thereby increasing the chance of a successful IVF.
Preparing and Retrieving the Eggs
Once your ovarian follicles are ready, a pregnancy hormone is injected in order for the ovaries to start preparing the eggs for maturation and ovulation. After this is done, the eggs are ready for retrieval. The physician will retrieve the eggs using ultrasound imaging in order to guide them in this intervention.
Egg Fertilization
The Laboratory team then exposes the eggs to sperm, which should lead to egg fertilization. At this stage, the embryos can either be transferred into your uterus, or frozen for transfer at a later date.
Embryo Transfer
The embryo (or, more rarely, multiple embryos) with the most chances to successfully implant is transferred into your womb. Usually, the time period between the egg retrieval and transfer is 5 days.
Pregnancy Testing
Two weeks after the transfer, you find out whether the implantation was successful. Once your pregnancy is confirmed, your team will closely monitor your situation, including your beta HCG levels and the embryo to make sure it is developing normally and implanted in the correct location in the uterus.

Accompanying Procedures to IVF
Intracytoplasmic Sperm Injection (ICSI)
In certain cases, the sperm is not able to penetrate the egg’s shell (which is the case in natural conception and IVF), for instance when the male patient’s sperm presents an abnormally low sperm count or sperm cannot be obtained without surgical techniques. The embryologist may then elect to perform an Intracytoplasmic Sperm Injection (ICSI), that allows them to inject a single sperm into a mature egg.
Percutaneous Epididymal Sperm Aspiration (PESA)
In cases where the male patient is not able to provide sperm naturally, the medical team can collect it from the epididymis using a fine needle. The procedure can be performed on a patient under local anesthesia, and the sperm collected must be used in an IVF procedure.
Testicular Sperm Aspiration (TESA)
TESA refers to a surgical technique used to collect a small sample of tissue from the testicle. TESA usually does not allow for retrieving enough sperm for freezing, but can be used if other sperm retrieval techniques are unsuccessful. After sperm is collected through TESA, it must be used in an ICSI.

